The enduring culture, deep spirituality, and unbreakable connection to Country define Aboriginal and Torres Strait Islander peoples as the First Peoples of Australia. Their continued existence, despite centuries of oppression, is a profound testament to their resilience and inherent strength. However, historical and ongoing trauma means that this community shoulders a disproportionately high burden of mental distress. This mental health platform is founded on the belief that healing must be culturally safe, respectful, and dedicated to addressing the unique and complex factors influencing the Social and Emotional Wellbeing (SEWB) of Aboriginal and Torres Strait Islander peoples. A genuine commitment to this community is paramount to fostering national healing and achieving equitable health outcomes across Australia.
The Profound Need for Culturally-Safe Support
For Aboriginal and Torres Strait Islander individuals, wellbeing is holistic—it’s about the whole self, which includes connection to:
- Spirituality and Ancestors
- Country and Land
- Culture, Language, and Kinship
Sadly, this foundational wellbeing is continually challenged by the enduring impacts of colonisation, dispossession, and assimilation policies. The most significant contributors to the disparity in mental health outcomes include the profound effects of intergenerational trauma (such as the forced removal of children during the Stolen Generations), which manifests as a complex legacy of grief and loss passed down through families.
Furthermore, experiences of systemic racism and discrimination in daily life, coupled with significant socio-economic disadvantages, act as chronic stressors that severely impact mental health. These factors result in Aboriginal and Torres Strait Islander adults reporting levels of psychological distress far higher than the non-Indigenous population.
Crucially, standard, mainstream mental health services frequently fail to acknowledge this deeper, holistic and historical context. They often lack the necessary cultural safety, leading to fear, distrust, and reluctance to seek help. Effective healing in an Australian context is thus achieved when support is delivered with respect, understanding, and cultural humility. Individuals deserve a space where their history, their identity, and their worldview are not just acknowledged but honoured.
Individuals seeking support can reach out to the confidential helpline today at 13 92 76 (13yarn.org.au).
Our Promise
At Intellect, we are deeply committed to walking alongside Aboriginal and Torres Strait Islander communities with genuine care. The commitment is built on these foundational principles:
- Honouring Culture: The platform recognises the incredible strengths within Aboriginal and Torres Strait Islander cultures, viewing them as powerful tools for healing. The approach is strengths-based, focusing on resilience and the inherent capacity for wellbeing.
- Trauma-Informed Care: Counsellors are trained to understand the pervasive impact of trauma, offering care that is gentle, non-judgmental, and respects an individual’s pace.
- Continuous Learning: The team is constantly working to improve its cultural competence, partnering with Indigenous experts to ensure services truly meet the needs of this group in a safe way across Australia.
PRESS RELEASE
Hong Kong, 2 July 2025 – Intellect and Prudence Foundation, the community investment arm of Prudential, are collaborating to launch Talk it Out, a mental health initiative in partnership with digital mental health service provider Intellect. Through the programme, communities in need in Malaysia and Vietnam will have access to free mental health support.
Talk It Out reflects Prudence Foundation’s commitment to building long-term health resilience by addressing mental well-being as a vital component of overall health, particularly as mental health emerges as a growing challenge in Southeast Asia. Around one in seven people in the region, equivalent to 260 million, live with a mental health condition. Many are also plagued by daily stress, burnout, relationship problems, and sleep issues. Barriers such as limited access to services, socioeconomic challenges, and financial constraints have resulted in widening gaps in mental healthcare in the region. In some countries, the treatment gap – defined as the percentage of individuals needing care but not receiving it – reaches up to 40 per cent.
Through the Intellect app, users will have access to a full spectrum of mental health services, including self-guided programmes, live consultations with licensed coaches, clinical psychologists and counsellors, and a 24/7 helpline that provides professional support in their local language. Where needed, users can also be connected to local mental health professionals for one-on-one coaching or counselling sessions, ensuring both scalability and personalised care for diverse community needs. To ensure accessibility and relevance to users in Malaysia and Vietnam, the app is available in multiple local languages such as Bahasa Malaysia, Chinese, Tamil, Vietnamese, French and English.
The programme will identify and engage vulnerable and at-risk groups in Malaysia and Vietnam, and work with local partners in healthcare, education, and community sectors. Talk It Out will be targeted to serve various local communities, including at-risk youth and women, low-income parents and families, marginalised and displaced communities. The programme will also be accompanied by targeted in-community workshops and awareness campaigns to help reduce stigma and equip users with essential knowledge.
Arjan Toor, CEO, Health, Prudential plc, said: “Our mission is to give our customers peace of mind by investing in and supporting initiatives that strengthen their ability to manage health challenges. Mental wellbeing is intrinsically linked with peace of mind, and enables people to lead resilient and meaningful lives. But there is a widening gap between the demand for mental health services and access to care, particularly within vulnerable communities. Through our collaboration with Prudence Foundation, we aim to end worry and hassle for people with a mental health condition. Launching this programme in two of our biggest health markets – Malaysia and Vietnam – is an important step forward in our commitment to helping our customers, and communities, when they need us most.”
Diana Guzman, Chair of Prudence Foundation and Chief Sustainability Officer, Prudential plc, said: “Our goal is to create meaningful, lasting change and build long-term health resilience. Across our markets, millions remain without health protection, not due to a lack of need, but because of affordability and access barriers. Mental health is a critical part of this equation. Without support for emotional and psychological wellbeing, individuals and families are left vulnerable to the pressures of daily life. That’s why we’re investing in targeted programmes like Talk It Out, which provide free, culturally relevant mental health support to those who need it most. By reaching vulnerable communities with accessible care, we’re not just filling a gap—we’re laying the foundation for stronger, more resilient lives.”
Theodoric Chew, CEO and Co-Founder, Intellect, said: “Our work with Prudence Foundation is a step towards building mental health resources and solutions that are universally accessible, especially for vulnerable and at-risk communities. By leveraging technology, our clinical expertise and on-the-ground networks, we are able to deliver meaningful care to those who need it most, in a way that’s scalable, localised, and sustainable.”
As a Tier 1 organisation in the 2025 CCLA Corporate Mental Health Benchmark, Prudential continues its commitment to supporting mental health wellbeing in the workplace and the community. For organisations interested to support their community’s mental health needs through this initiative, please contact [email protected]
END
About Prudential plc
Prudential plc provides life and health insurance and asset management in 24 markets across Asia and Africa. Prudential’s mission is to be the most trusted partner and protector for this generation and generations to come, by providing simple and accessible financial and health solutions. The business has dual primary listings on the Stock Exchange of Hong Kong (2378) and the London Stock Exchange (PRU). It also has a secondary listing on the Singapore Stock Exchange (K6S) and a listing on the New York Stock Exchange (PUK) in the form of American Depositary Receipts. It is a constituent of the Hang Seng Composite Index and is also included for trading in the Shenzhen-Hong Kong Stock Connect programme and the Shanghai-Hong Kong Stock Connect programme.
Prudential is not affiliated in any manner with Prudential Financial, Inc. a company whose principal place of business is in the United States of America, nor with The Prudential Assurance Company Limited, a subsidiary of M&G plc, a company incorporated in the United Kingdom.
About Prudence Foundation
Established in 2011 in Hong Kong, Prudence Foundation is the community investment and philanthropic arm of Prudential plc.
The Foundation builds financial wellbeing, and climate and health resilience for underserved Asian and African communities. We are committed to sustainable, long-term solutions that empower individuals and communities to make informed financial decisions, access affordable financial products, as well as be more prepared and protected against climate related health risks. We actively engage in public-private partnerships, collaborate with governments, NGOs, communities and other private sector entities to build collective efforts for lasting change. To date, our programmes are implemented across 16 markets in Asia and Africa, reaching millions of people.
For more information: www.prudencefoundation.com
About Intellect
Intellect is a trusted global leader in mental health care, providing accessible, culturally-localised support through comprehensive solutions that address diverse needs at every stage of the mental health journey. Available in 120+ languages, Intellect’s comprehensive local network of providers is accessible in 100+ countries. Online and offline, it has made a difference in the lives of over 4 million users around the world.
Intellect is backed by influential investors including Tiger Global, Insignia Ventures Partners, Y Combinator, HOF Capital, MS&AD Ventures, and East Ventures, alongside prominent venture funds, family offices, big tech executives, and angel investors. In 2025,
Intellect was named as one of Fast Company’s Most Innovative Companies and Human Resources Online’s Best Digital Wellness Platform (Gold) in 2023.
]]>For insights to be useful, data must be timely. Otherwise, you’d be solving issues that have already evolved or been replaced. But even with fresh numbers, translating them into action can be hard without the right context and guidance.
That’s why we designed Intellect Vault as one of Intellect Atlas’ Artificial Intelligence (AI) capabilities: to help HR professionals stay ahead of emerging stressors and turn data into action using best practices.
Disclaimer: You might not see all the features below yet as Intellect Vault is currently being piloted with select clients, but they’re well on their way.
What is Intellect Vault?
Intellect Vault gives HR professionals a live view of how their people are truly doing. The data is not only more timely but also deeper, drawing from sources such as:
- Self-reported check-ins
- Platform engagement patterns
- Interactions with Intellect’s coaches and clinicians
All data is anonymised and aggregated, ensuring complete protection of user privacy and confidentiality at every stage. These real-time, high-quality insights empower HR teams to act on trusted, measurable recommendations that drive real results.
To achieve this, Intellect Vault was purpose-built to be your:
1. Insights Engine
In fast-moving workplaces, data and insights can quickly lose their relevance, and recommendations often become outdated by the time they’re implemented. So HR teams get stuck in “firefighting” mode, reacting to old problems instead of proactively addressing new ones.
How does Intellect Vault change that?
Intellect Vault acts as an early warning system, surfacing risks in real time. It includes:
- Insights Dashboard: Allows HR teams to explore and analyse data independently.
- Insights Chatbot: Answers HR’s questions instantly, simplifying data interpretation.
- HR Pulse Emails: Quarterly reports featuring bite-sized insights and actionable recommendations.
What does this mean for HR? HR teams no longer waste time crunching numbers while leaving issues to escalate. Staying on top of red flags like stress and burnout, they can respond proactively before they impact the bottom line.
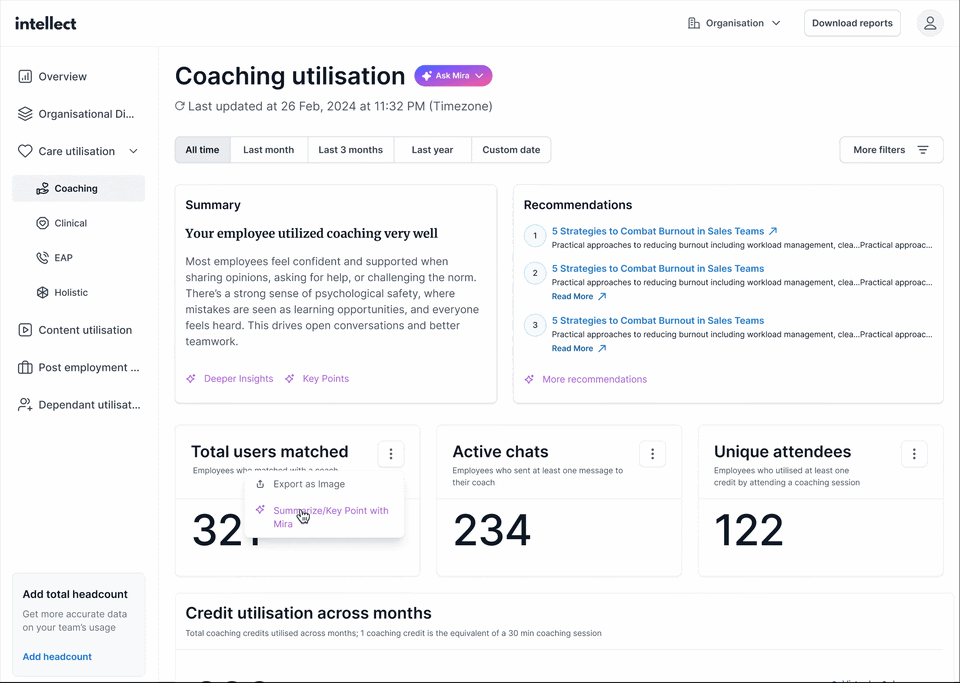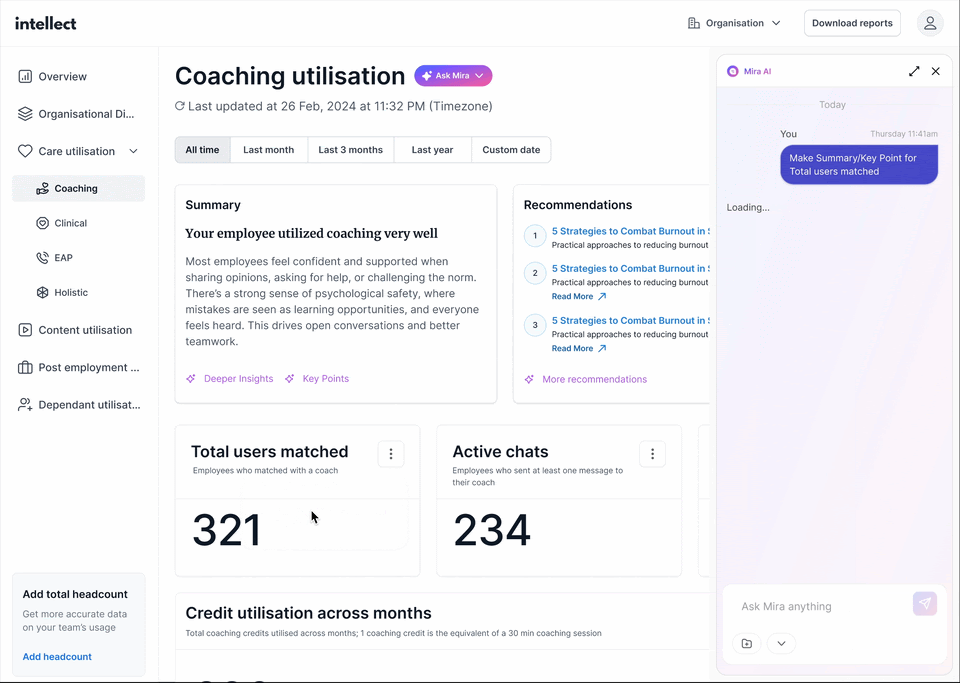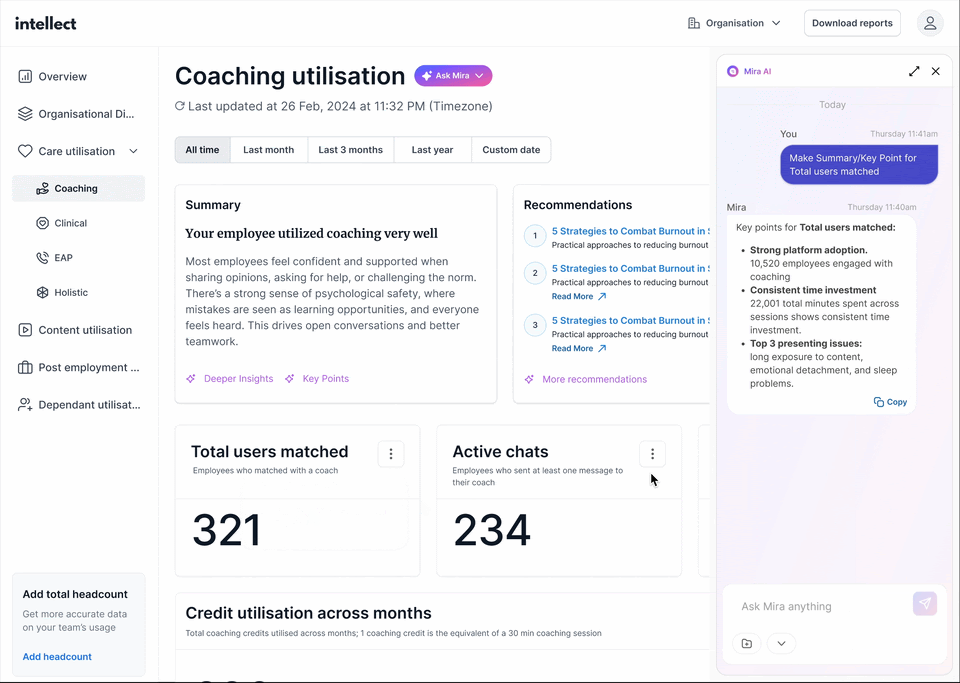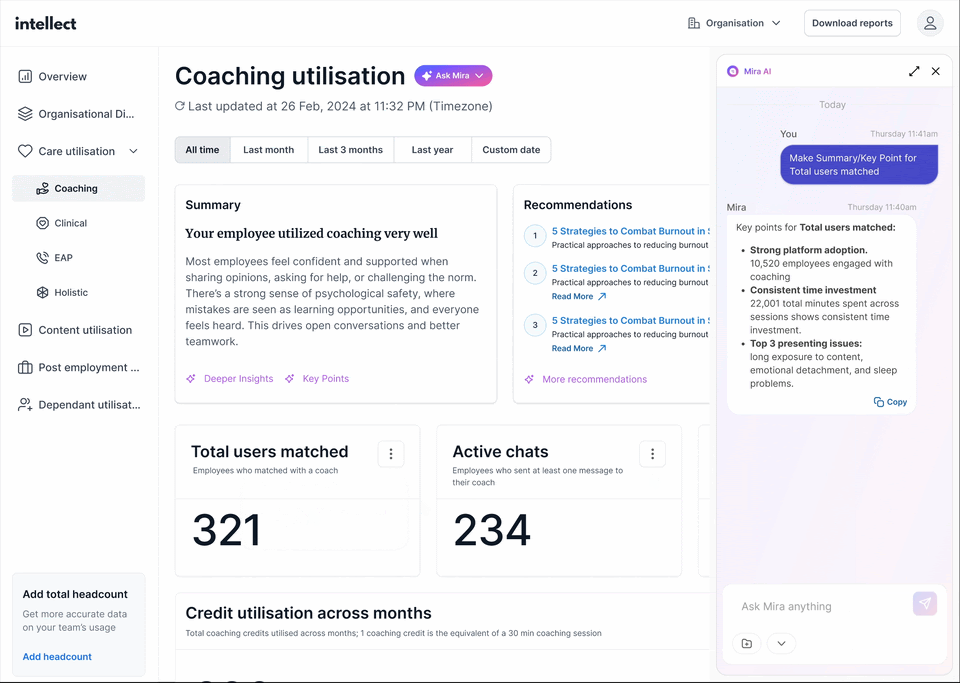
2. Decision Enabler
Data is only as powerful as the action that follows, but the next steps aren’t always clear for HR teams. Often, it becomes a process of trial and error, testing different interventions and hoping something sticks.
How does Intellect Vault change that? Based on the insights, Intellect Vault recommends individual and systemic interventions via the Insights Dashboard and through HR Pulse Emails.
For example, if Intellect Vault detects a 20% rise in reported stress levels alongside a dip in Employee Assistance Programme (EAP) usage, it might suggest reviewing work-life balance policies or increasing awareness of available support resources during high-stress periods.
What does this mean for HR? Less time is spent debating next steps, and more on implementing best practices refined through Intellect’s partnerships with over 200 organisations. Solutioning is faster and results-oriented, making HR more efficient and effective.
3. Impact Tracker
Employee wellbeing is the strongest predictor of productivity, but it’s often seen as a “nice to have” because proving its impact is difficult. How do we attribute improvements in performance to our wellbeing initiatives?
How does Intellect Vault change that? Intellect Vault closes the loop by measuring the outcomes of its recommendations. It tracks wellbeing trends and connects them to performance-related metrics, helping highlight what’s working and what needs attention.
What this means for HR: Improvements in outcomes like productivity can be measured and even translated into financial impact. This equips HR with the data they need to refine strategy and build a compelling case for continued investment in employee wellbeing.
Role of Client Success Managers
You might be thinking: Isn’t HR, at its core, a human discipline? You’re absolutely right. AI can show what is happening, but it’s professional judgment and contextual knowledge that explain why.
For example, AI might detect rising stress levels and declining EAP usage, but it won’t know how to connect those trends to an intense product release cycle, where your engineers are currently on a 24/7 on-call rotation.
That’s why Intellect Vault is designed to complement, not replace, your HR professionals and Intellect’s Client Success Managers (CSMs).
What Intellect’s CSMs do:
- Validate AI signals by checking sprint schedules to confirm if team members are really too busy to book sessions.
- Contextualise trends with historical and organisational factors. Were stress levels similar last year? Is the recent restructuring a contributor?
- Offer practical recommendations that fit your situation, such as
- Sharing asynchronous resources employees can use anytime
- Sending reminders about helpful tools through newsletters or chat
- Running stress management workshops for certain teams
Intellect Vault kicks off strategic dialogues with our CSMs, who serve as trusted advisors who can help HR professionals make sense of the data and act on it.
Combining artificial and human intelligence
Ultimately, it is this synergy between artificial and human intelligence; algorithmic precision and human insight that powers Intellect Atlas, an AI layer that transforms how organisations, individuals and clinicians experience mental healthcare.
]]>Bullying, harassment, and aggression are among the psychosocial hazards that are becoming increasingly prevalent in Australia. In Victoria, work-related mental injuries accounted for 18% of all new WorkCover claims in 2023 to 2024, up from 16% the year before, and just 9% prior to 2009.
The good news, though, is that change is already underway.
Psychosocial hazards Victoria: What’s coming in 2025
Australia’s evolving Work Health and Safety laws are set to place psychosocial hazards on equal footing with physical ones.
- 2021: Safe Work Australia released the Model Code of Practice on Managing Psychosocial Hazards at Work, alongside the introduction of ISO 45003, the international standard for managing psychological health and safety.
- 2022: The Work Health and Safety Amendment Regulation 2022 further advanced this shift by formally incorporating specific requirements for managing psychosocial risks.
- Q4 2025 (Coming soon): The Victorian Government is expected to announce new regulations in October, with implementation scheduled for December. Once in place, every Australian jurisdiction will have formalised regulations targeting the management and control of psychosocial hazards.
According to the consultation draft, Victoria’s upcoming regulations aim to provide employers with clearer guidance on identifying and managing psychological hazards at work. This includes the introduction of a compliance code to support implementation.
With these changes on the horizon, now is the perfect opportunity to strengthen your workplace culture. Partners like Intellect can help you go beyond compliance and build psychological safety that drives engagement, performance, and long-term business success.
What are psychosocial hazards?
Put simply, psychosocial hazards are the psychological stressors that emerge from a person’s social and workplace environment. These risks often have deeper, systemic roots—such as toxic leadership—making it essential for organisations to tackle the underlying causes rather than just treating the symptoms.
Imagine that you are working under a manager who publicly humiliates you for speaking up in meetings or who makes inappropriate remarks about your appearance. Even in an office that meets all physical safety standards, such experiences can put you in a constant state of fight, flight, or freeze.
The consequences go beyond diminished work performance, as chronic exposure to psychosocial hazards can seriously undermine mental health, leading to conditions like anxiety, depression, Post-Traumatic Stress Disorder (PTSD), and sleep disorders.
While psychosocial risks like bullying and harassment are overt, others are more subtle. Below are the 17 psychosocial hazards identified in Managing Psychosocial Hazards at Work Code of Practice 2024.
Psychosocial hazards examples
- Job demands
- Job insecurity
- Low job control
- Fatigue
- Poor support
- Lack of role clarity
- Poor organisational change management
- Inadequate award recognition
- Poor organisational justice
- Traumatic events or material
- Remote or isolated work
- Intrusive surveillance
- Poor physical environment
- Violence and aggression
- Bullying
- Harassment including sexual harassment
- Conflict or poor workplace relationships and interactions
Psychosocial hazards in the workplace can arise from different aspects, such as:
- The design or management of work: An employee working remotely may experience low job control when constant keystroke monitoring limits their autonomy.
- The work environment: A social worker conducting home visits may be exposed to violence and aggression when supporting clients in domestic violence situations.
- Plant at a workplace: A machine operator may experience fatigue when required to maintain intense focus for long hours without adequate breaks.
- Workplace interactions or behaviours: A whistleblower may experience poor organisational justice when their identity is disclosed despite assurance of confidentiality.
Managing psychosocial hazards at work
How do we prevent psychosocial hazards in the workplace? Under the framework of the Workplace Health & Safety (WHS) Act 2011, compliance involves a structured, four-step process.
1. Psychosocial risk assessment: Start by conducting a comprehensive psychosocial risk assessment across the organisation to identify gaps.
2. Psychosocial risk report: Create a report comprising findings and recommendations, ranging from eliminating specific psychosocial hazards to redesigning workflows and adjusting policies.
3. Intervention implementation: Implement targeted interventions that minimise psychosocial hazards and enhance mental health outcomes.
4. Monitor, control and evaluate: Establish a system to monitor, control and evaluate their effectiveness and continue flagging psychosocial hazards.
Understandably, this process can feel overwhelming for employers—and that’s where we come in. Aligned with ISO 45003 framework, Intellect functions as a primary, secondary and tertiary intervention all in one.

Trusted by some of the world’s largest companies and over four million members globally, we address risks before they arise, mitigate them when they do, and support recovery when harm occurs.
How Intellect manages psychosocial hazards in the workplace
1. Primary: Intellect Consulting
As a primary intervention, Intellect Consulting focuses on organisational-level controls that eliminate or reduce psychosocial hazards. Our 4-phase framework is perfectly aligned with the compliance stages outlined in regulations, integrating diagnosis, design, implementation and measurement into one cohesive journey.

Phase 1: Diagnostics and Gap Analyses
We begin by using Intellect’s Psychosocial Risk Assessment & Consulting tool to evaluate psychological risk levels across your organisation. Our tool accounts for validated dimensions such as:
| DOMAIN | ITEM (ADAPTED FROM) |
| Workload & demands | – I have too much time to do in the time I’m given. (COPSOQ II, WHSQ) – I often feel emotionally drained at work. (COPSOQ II, ISO45003) |
| Job control | – I have little say over how I do my work. (HSE, WHSQ, JCQ) – I rarely get to decide when to take breaks. (HSE) |
| Role clarity | – I’m unclear about what’s expected of me in my role. (COPSOQ II, WHSQ) |
| Support | – I can rely on my manager if things get rough. (COPSOQ II, WHSQ) – My team supports each other when someone is struggling. (COPSOQ II) |
| Recognition & fairness | – I feel my work is recognised and appreciated. (ERI, COPSOQ II) – Decisions here are made fairly and transparently. (COPSOQ II, WHSQ) |
| Change management | – I’m kept informed during changes that affect my work. (HSE, ISO45003) |
| Workplace relationships | – I’ve experienced or witnessed disrespectful behaviour at work. (WHSQ, NOM-035) – People in my workplace treat each other with kindness and respect (COPSOQ II, WHSQ) |
| Work-life balance | – Work often interferes with my personal or family life. (COPSOQ II, WHSQ) |
If your organisation is already on Intellect EAP, that’s perfect. We can incorporate that data to deliver a more complete picture of your organisation’s risks.
Most importantly, it allows you to pinpoint specific roles, teams, and locations where risks are the most prevalent, setting the stage for Phase 2.
Phase 2: Strategy and Solution Design
Based on our findings, our Organisational Wellbeing Consultancy team will design interventions to address specific psychosocial hazards. This isn’t about offering quick fixes, like generic mindfulness sessions, but embedding wellbeing deeply into your leadership, culture, and policies.
Phase 3: Implementation and Intervention
Our consultancy team doesn’t just flag problems, we partner with you to solve them. In close collaboration with Work Health and Safety leaders, we ensure every control implemented is tied to a measurable reduction in risk exposure.
Here are some evidence-based strategies we may use to address the psychosocial hazards identified in your organisation.
| PSYCHOSOCIAL HAZARD | CONTROL |
| Change management | Leadership: Executive coaching to manage transitions (e.g. organisational restructuring) more smoothly |
| Poor support | Culture: Managerial coaching to support healthy team dynamics and Mental Health First Aid (MHFA) training to establish a peer support network |
Job control | Policies: Flexible work arrangements to increase employee’s autonomy over working hours and locations |
Phase 4: Post-intervention Evaluation
After the interventions have been in place for some time, we track their impact on key outcomes ranging from employee wellbeing to productivity. To simplify this process, our Intellect Echo tool:
- Administers psychosocial risk assessments and pulse surveys
- Accelerates insight generation for leaders to respond quickly and confidently
- Enables ongoing compliance reporting for regulators and internal WHS audits
2. Secondary: Intellect EAP
As a secondary intervention, Intellect EAP strengthens employee resilience by equipping employees with resources to manage stressors before they escalate.
Unlike traditional EAPs with wait times of up to three weeks, Intellect connects employees to care in an average of just 24 hours (1.04 days). The breadth of our offerings also ensures that support is not just reactive but preventative, addressing psychosocial risk in a timely and effective manner.
| PSYCHOSOCIAL HAZARDS | PRODUCT/SERVICE |
| Workplace relationships | Intellect Proactive Self-care resources on topics like boundaries and conflict resolution help with navigating interpersonal challenges. |
| Role clarity | Intellect Coaching Professional guidance hones communication and self-advocacy skills that empowers one to articulate their needs. |
| Job insecurity | Intellect Holistic Financial coaching supports employees facing monetary challenges in moving from distress to an action-focused mindset. |
| Traumatic events or material | Intellect Care Clinical-grade psychotherapy offers evidence-based treatments for conditions such as PTSD. |
| Workplace harassment | Intellect Helpline Trained professionals support employees in moments of acute distress while safeguarding their anonymity. |
*Intellect Care and Intellect Helpline also function as tertiary interventions by reducing the harmful effects of exposure to psychosocial hazards.
3. Tertiary: Intellect Specialised Care
As a tertiary intervention, Intellect’s Return to Work programme functions as a rehabilitation system that supports employees in regaining their mental health and workplace functioning.
Imagine a content moderator who has been directly exposed to traumatic material, diagnosed with PTSD, and has taken time off to recover. After a few months, how do you determine whether they’re ready to resume regular duties? Does that mean diving back in immediately? And how do you communicate this transition to their manager and peers?
Our Return to Work programme was designed with this reality in mind, helping employers:
- Assess psychological readiness to return: Clinical psychologists with experience in return-to-work assessments and rehabilitation planning evaluate the employee’s readiness to re-enter the workplace.
- Provide expert recommendations for employees and employers: Flexible work arrangements allow employees to meet their mental health professionals during office hours, ensuring treatment continuity without added stress.
- Create a supportive environment for sustainable reintegration: Quarterly coaching sessions help managers and peers who work directly with the returning employee become effective allies.
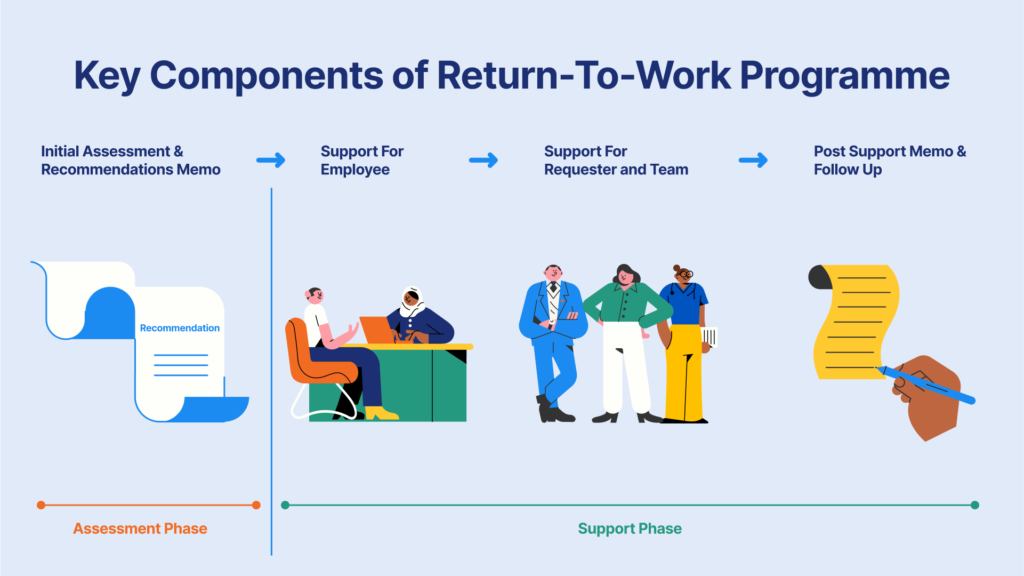
Paired with ongoing support through Intellect EAP, a structured reintegration plan acts as a safety net, empowering affected employees to build resilience and return with confidence.
Keeping psychosocial hazards in check
Did you know that mental wellbeing is the strongest predictor of employee productivity? That’s why leading firms are embedding psychological safety into their core strategy instead of treating it as an afterthought.
This also means that psychosocial hazards aren’t just an HR issue; they’re an enterprise-wide concern with significant implications for business performance. Employers who address these risks proactively don’t just stay compliant; they outperform with higher retention, improved morale, and fewer incident claims.
Book a demo today and start building a safer, healthier, and more productive workplace.
]]>But ask anyone who’s benefited from a good therapist, and they’ll tell you: human presence makes a difference. Sometimes it’s subtle, non-verbal signals—like a knowing nod—that invite deeper sharing. Other times, it’s the solace found in a moment of silence as a therapist simply witnesses a client’s pain.
Healing isn’t just about finding answers. It’s about our shared humanity, which is something technology can’t replace. As we scale AI mental health tools, the real question is this: What should humans still own and where should AI take the lead?
What AI can do and what it can’t
A 2024 study found that AI-driven chatbots reduced depressive symptoms in over 70% of low-risk users, rivaling human coaches. In some areas, like coaching, check-ins, or early-stage student support, a human may not need to be in the loop at all. Automation allows these services to scale and reach more people than ever before.
However, automation often falls short in other domains. In high-stakes situations requiring trauma-informed care or acute risk intervention, AI may never match the nuance and expertise of licensed professionals. In some cases, its echo chamber effect can even make things worse.
Here’s what we think AI does better, and what humans still do best:
What AI does better
- Triage and risk escalation: AI doesn’t get tired. It never forgets to ask. It isn’t swayed by bias or fatigue. Early trials suggest AI can flag risk faster than human intake teams—potentially catching warning signs before they escalate.
- Data-driven matching and insights: AI can learn from thousands of sessions, surfacing care patterns and provider matches that might go unnoticed by humans. For example, it can match patients with therapists based on personality traits and past treatment outcomes.
- Admin, summaries, and prep: Clinicians shouldn’t spend half their time on notes, scheduling, or follow-ups. AI can shoulder the administrative load, freeing up time and energy for what matters most: the patient.
What humans still do best
- Ethical judgement: Humans understand when rules should be followed and bent. For example, a clinician may decide, after assessing that a client is risk of harm to others, to breach confidentiality and alert an emergency contact.
- Cultural intuition: Humans can grasp context that AI can’t, even with data. When an Asian client says, “It’s just stress, I’m used to it,” a clinician attuned to cultural norms may hear what’s unsaid and gently uncover the hidden burden beneath.
- Reframing and resonance: Humans can hold space for ambiguity, contradiction, and even silence. When a client says, “I don’t know if I want to get better,” a clinician can hold space for their ambivalence without defaulting to problem-solving mode.
- Relational depth: When words fail, human connection can be healing. Without offering advice of any sort, a clinician may sit quietly with a grieving parent, providing a steady presence that makes them feel less alone.
Based on the strengths of artificial and human intelligence, we need to clearly define where AI should lead, where it should support, and where it should step aside entirely. That might look like:
| Care mode | Best used when: | Examples |
| Fully AI-led | Low risk, low emotional depth. Task-focused and available 24/7. | – Skill-building exercises – Habit tracking – Psychoeducation – Automated nudges |
| AI-led with human oversight | Moderate emotional load. High-frequency support that may need escalation. | – In-care check-ins – Human in the loop chats – Treatment adherence – Support groups |
| Human-AI collaboration | Precision needed. AI offers insights; human makes care decisions. | – Diagnostic assessments – Treatment planning – Medication reviews – Care coordination |
| Human-led with AI support | High emotional risk or ambiguity. Trust and context matter most. | – Complex grief – Cultural navigation – Trauma-informed therapy – Family therpay |
| Human-led only | Acute crisis or ethical complexity. Requires full human presence. | – Suicide prevention – Abuse disclosures – Crisis intervention – Ethical dilemmas |
With Intellect Atlas, we’re using AI to:
- Recommend care types and surface needs before a session
- Draft case summaries to free up therapist time
- Support users who may never want or need a human provider
Intellect Atlas’ approach to AI mental health
Did you know that the therapeutic alliance, which is the bond between clinician and client, is the strongest predictor of treatment outcomes in mental healthcare?
At Intellect, we aim to expand access to our platform while preserving the human touch that drives meaningful treatment outcomes. So, in bringing Intellect Atlas to life, we found ourselves asking:
Where does human judgment lead to better outcomes?
Where can automation reduce friction—without reducing empathy?
Where does human presence (or its absence) shape how safe someone feels?
Crucially, where might this experience go wrong?
These aren’t theoretical questions. They’re product questions. Design questions. Roadmap questions. And as the product and design lead at Intellect, we have to make sure we get it right. Because if we don’t, people can get hurt.
The future of AI mental health is hybrid
The next decade of care won’t be AI-first or human-first. It will be value-first.
It’s not AI versus humans, it’s about knowing when to lean on each. Sometimes AI leads, sometimes a human does. The key is knowing when.
Unlike most narratives surrounding AI, this isn’t about “protecting” jobs. It’s about preserving human touch, values, and judgment across every layer of care—while ensuring both scalability and quality. (We call it hospital-grade delivery and service.)
That’s what we’re really building for.
More than just a chatbot, Atlas is an artificial intelligence (AI) layer that permeates every touchpoint of the Intellect experience. For individuals, organisations and clinicians, Atlas introduces a new era of AI mental healthcare—smarter, faster, and more scalable than ever before.
Powering safe, intentional, and highly attuned mental healthcare
We didn’t design Intellect Atlas to replace licensed professionals, but to partner them in delivering safe, intentional and highly attuned mental healthcare.
Safe: Intellect Atlas is built for safety. Intelligence and trust go hand in hand. With enterprise-grade security and strict data residency protocols, Atlas ensures users have both confidence and complete control over their data. And as our AI agents work alongside licensed professionals, every aspect of care is clinically validated.
Intentional: Intellect Atlas is intentional. Repeating your story at every appointment shouldn’t be the norm—it’s a sign of fragmented, outdated systems. More than just a chatbot or AI plug-in, Atlas connects users, care teams, and organisations through an integrated platform that enhances the quality, speed, and scalability of mental healthcare.
Highly attuned: Every mental health journey is unique, and our AI learns from each user’s interactions, background, and changing needs to deliver care that’s truly personalised. By meeting users where they are in real time, Atlas provides relevant support that drives better outcomes for individuals and organisations worldwide.
Guided by these principles, we’re excited to introduce Intellect Guardian, Intellect Vault, and Intellect Cruise.
A new era of AI mental health
Intellect Guardian: Your Personal AI Care Companion for Always-On Support
Intellect Guardian is a network of AI agents that delivers personalised mental health support round the clock. Each agent brings deep domain knowledge, forming an all-rounded taskforce built just for you.

Meet your A-team:
- Chat Companion: As soon as you’re onboarded, our adaptive AI chatbot begins building your care profile through interactions, assessments, and analysis. It’s not a static snapshot, but a living, breathing portrait of who you are.
- Care Navigator: Not sure whether you need a coach, counsellor, or clinical psychologist? Our AI-powered intake and triage tool removes the guesswork by assessing your needs in real time and guiding you to the right level of care.
- Self-care Partner: Like telepathy, our self-care AI assistant generates journaling prompts and handpicks resources that speak directly to what you’re facing, just in case you need a little support between sessions.
- Holistic Care Team: Beyond mental wellbeing, our AI-powered multidisciplinary care team supports key areas of your lifestyle, including nutrition, sleep, fitness. The “avengers” of total wellbeing have all your bases covered.
- 24/7 Distress Support: What should I do if I can’t sleep? Am I having a panic attack? Consider our always-on AI support system an emotional A&E department, offering immediate relief and escalating to human support when necessary.
Intellect Vault: Your AI Intelligence Engine for Smarter Wellbeing Insights
The insights from Intellect Guardian and Intellect Cruise culminate in Intellect Vault, an AI-driven dashboard that delivers real-time trends, risk signals, and next steps directly to your inbox. Having access to your vitals at all times enables smarter, faster decision-making.

Meet your new HR partner:
- Insights Engine: Goodbye quarterly surveys and static spreadsheets. Our AI-powered system offers real-time insights into your workforce’s wellbeing, allowing you to address disengagement before it impacts performance or retention.
- Decision Enabler: Our automated emails don’t just tell you what’s wrong—they help you fix it. From boosting EAP visibility to implementing workload management strategies, our recommendations are grounded in data.
- Impact Tracker: Our summarised reports connect wellbeing data to key performance outcomes, like productivity, and track them over time so know what’s working and what isn’t.
Intellect Cruise: AI Healthcare Assistant for More Impactful Care
Intellect Cruise is an AI assistant designed for clinicians, reducing their administrative burden and freeing up more time for what truly matters: connecting with their clients and delivering person-centred care.

Meet your new PA:
- Automated Intelligent Provider Workflows: Let Atlas handle the paperwork. Our AI-driven workflow automation streamlines everything from appointment scheduling to space booking so clinicians can concentrate on improving patient care and treatment outcomes.
- Scalable Healthcare Operations Intelligence: Our AI-powered system looks at provider schedules and no-show trends to optimise resource planning and provider efficiency. Plus, it improves collaboration and provides real-time insights.
- Continuous Patient Support: From check-ins to symptom tracking, our AI-powered engagement and monitoring tools help clinicians stay on top of their cases, enabling timely intervention as well as treatment adherence and continuity.
Bringing the best of both worlds
How can we use AI as a force for good? Unlike in sectors such as e-commerce or education, this question looms large in the mental health space, where data is deeply personal and the stakes incredibly high.
With Intellect Atlas, individuals, employers, and healthcare providers can maximise the potential of AI while minimising uncertainties, proving that mental health services can be both high-tech and human-centric.
]]>Talk about incorporating AI in healthcare and the usual buzzwords are speed, scale and efficiency. But mental health is a different ball game. Unlike sectors like e-commerce or food delivery, it touches the most sensitive parts of a person’s life: their relationships, their trauma history, their emotional resilience. Here, AI therapy gone wrong isn’t just an inconvenience. It can be seriously harmful.
Why AI therapy can be risky
Misdiagnosis
Unlike a wrong product recommendation or a late food delivery, the wrong response doesn’t just cause frustration to a vulnerable user. It can cut very deep to their identity and self-worth, leaving them feeling even more distressed than before.
Consider a coaching client of mine. When she told an AI platform she felt “overwhelmed,” the chatbot labeled her with “anxiety.” But it missed the bigger picture: her perfectionistic tendencies and the unique pressures she faced at work, which should have been considered before conclusions were made. A couple of weeks later, she internalised this response and started seeing herself as “an anxious person.”
Unfortunately, this is how most AI platforms operate. Generic symptom checkers and chatbot scripts can overlook subtle cues in language, emotion and context that are critical to providing the right care. This is somewhat expected, since they’re not designed specifically for mental health. That is why AI therapy must follow a different playbook; one that is centered on trust, safety, and ethics.
Unchecked bias
When we rely on AI therapy, the risks go far beyond simple misinformation. Unchecked bias, which can distort reality by reinforcing one’s beliefs rather than challenging them, is equally precarious.
This issue is not new. Social media platforms have long demonstrated how algorithms pander to emotions like anger, insecurity, and isolation instead of promoting balance. Netflix documentaries like The Social Dilemma and, more recently, Adolescence, illustrate this perfectly.
Now, imagine how this plays out when we turn to AI therapy. The echo chamber effect is practically on steroids. We’re talking about the reinforcement of toxic self-narratives, feelings of helplessness, or even a false sense of confidence—each of which can further deepen isolation.
Unchecked bias doesn’t just affect individuals. Left unchecked, it can reshape entire societies. Just look at the impact social media has had, both for better and for worse. This is why mental health companies must design their AI systems with this reality in mind from day one.

“But AI makes me feel seen and heard.”
To understand why unchecked bias can be problematic in mental healthcare, we must acknowledge this: A therapist who spends most sessions nodding along in agreement may be validating, but they’re not necessarily being effective.
On my journey to becoming a behavioural health coach, one of the most important lessons I learned is that real support isn’t about affirming everything someone says. It’s about helping them uncover subconscious patterns and challenge long-held beliefs, thereby opening up space for growth.
One of my favourite techniques, for instance, is simply asking clients: “Is that necessarily true?” This small but powerful question encourages them to examine their assumptions, rather than just having them reflected back without a shred of critical thought. Yet, that’s what generic AI chatbots do most of the time.
Rules for responsible AI therapy
AI therapy cannot just be a friendly mirror. It needs to be an ethical guide that nurtures and challenges users judiciously. As such, it cannot be built for engagement, it needs to be built for outcomes.
Here are five principles we believe should guide the development of AI mental health tools, and that shape how we approach AI at Intellect.
- Contextual awareness: AI therapy should be able to distinguish fleeting emotions from persistent patterns and adapt their response accordingly. When a statement like “I’m feeling anxious about my presentation tomorrow” is misconstrued as “I’ve been experiencing anxiety daily for months,” the response generated can do more harm than good to users, like it did my client.
- Challenging, not just validating: AI therapy should validate emotions while challenging unhelpful patterns of thought and behaviour. For instance, a response like “It’s natural to feel this way AND I wonder if there’s another way to look at this situation?” shows empathy while modelling cognitive flexibility.
- Clear handoff protocols: AI therapy should not replace licensed mental health professionals, and must incorporate clear triggers for escalation to human support. These should be based on severity indicators, such as suicidal ideation or signs of abuse, as well as patterns that suggest worsening mental states, like a user becoming increasingly stuck in negative thinking despite interventions.
- Cultural competence: AI therapy need to be built with cultural context at its core. A Southeast Asian user might say, “My heart feels heavy”—a common expression of distress that a Western-trained model could easily miss. As emotional vocabulary varies across cultures, developers must include diverse training data and perspectives or risk misinterpreting or overlooking critical signs.
- Transparency about limitations: Last but not least, users of AI therapy should always know they’re speaking with a chatbot, understand its limitations, and be directed to licensed mental health professionals where necessary.

Efficient and ethical AI therapy
These five principles may seem demanding, especially for teams focused on rapid development and market reach. However, they don’t have to slow progress. In fact, they can often accelerate long-term success. There’s a common myth that ethics hinders innovation, but that doesn’t have to be the case.
When we design for transparency, fairness, and human dignity from the start, we unlock deeper engagement, greater trust, and—most importantly—better outcomes. Users are more willing to open up. Clinicians are more willing to collaborate. Organisations are more willing to integrate.
As we build the future of mental health care, we have a choice: we can use AI to automate services, farm engagement and simply echo users’ thoughts, or we can use it to build trust, strengthen human connection, and offer real hope to those in search of it.
]]>